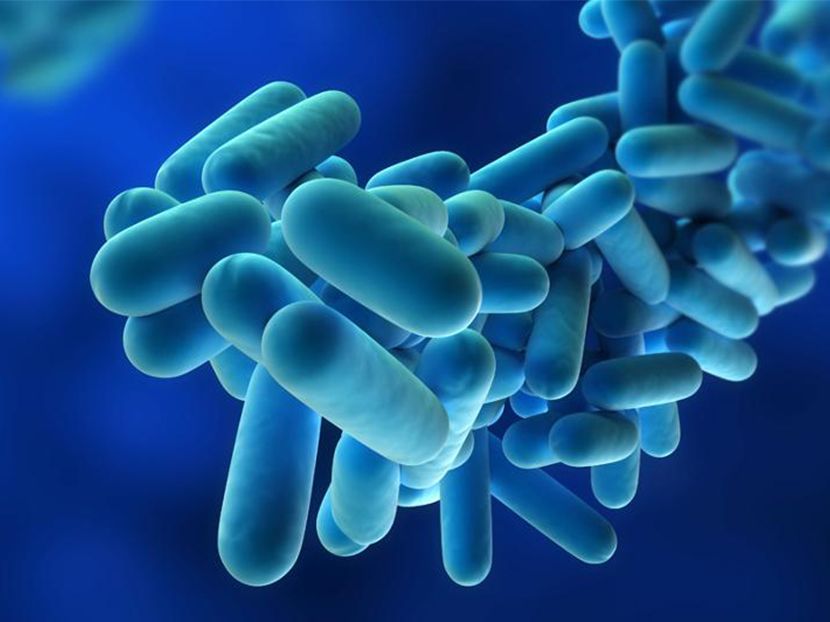
Legionellosis, also known as legion fever or legionella pneumonia or legionnaires’ disease, is a mild febrile to a serious and sometimes a fatal form of atypical pneumonia resulting from a bacterial infection. This waterborne disease is caused by exposure to any bacteria of the Legionella species that is found naturally in the freshwaters and in potting mixes. Based on the type of exposure, it can be categorized as travel, hospital or community acquired.
The number of global cases are unknown. It is estimated that about 2-9% Legionellosis cases are due to pneumonia acquired outside the hospital. Nearly 8,000-18,000 of its cases each year in the US require hospitalization. The outbreaks of the disease lead to minority of cases. Though it more commonly occurs during the fall and summer, it can occur around the year.
The first outbreak of Legionnaires’ disease was identified in 1977 as a severe pneumonia took place in the 1976 American Legion convention in Philadelphia. The disease is believed to have been named after this outbreak.
Now know about the causes, symptoms, diagnosis and treatment of the disease here.
Causes & Risk Factors
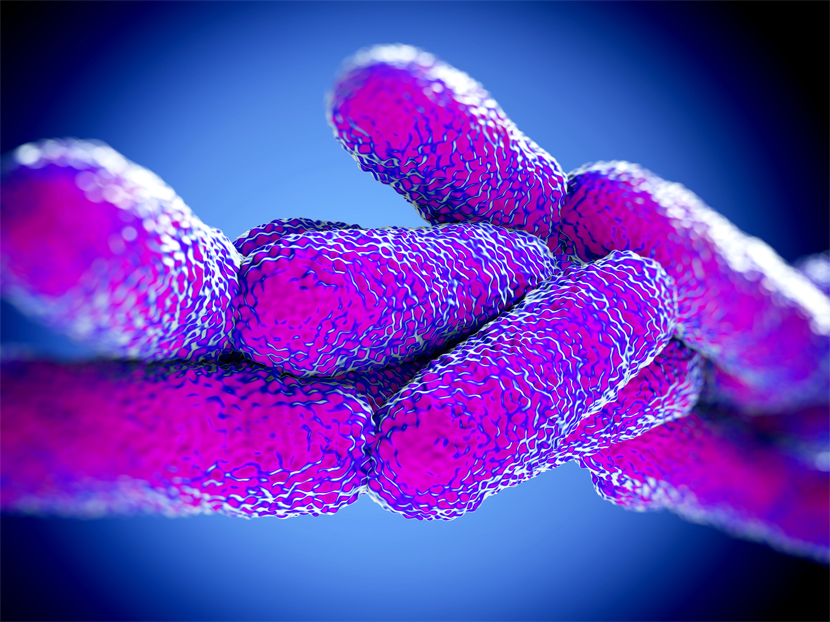
The major causative agents of Legionellosis are the species of Legionella bacteria found in the freshwater bodies (where it naturally occurs) and potting mix. L. pneumophila that is a widely found freshwater species in the natural aquatic environments is the most common cause of the illness.
However, the artificial water systems providing environments conducive to the growth and dissemination of Legionella are the most probable sources of the disease. The bacteria thrives and grows within the free-living protozoa and inside biofilms in the water systems at temperatures of 20-50 degrees Celsius. They can lead to infections by contaminating the human cells with the help of a similar mechanism used for infecting the protozoa.
The hot water tanks, hot tubs, humidifiers, whirlpool spas and cooling towers of big ACs can get contaminated by the bacterium. It is mostly spread through breathing in mist containing bacteria. When the aspirated water or ice is contaminated, the illness can take place. The disease does not spread directly between the most of the people who are exposed don’t get infected.
The risk factors for the infection are people who have history of smoking, chronic lung disease, old age, and poor immune function. It is also recommended that people suffering from severe pneumonia and those with pneumonia and travel history be tested for the presence of legionellosis.
Signs & Symptoms

It usually takes 2-10 days within exposure of bacteria for the symptoms to appear. And in rare cases, it may even go upto 20 days. The people affected by the disease usually experience fever, cough (dry or with sputum) and chills. Almost every infected individual has fever, nearly half of the people have cough with sputum and about one-third have cough with bloody sputum.
Some of the people may also experience diarrhea, vomiting, tiredness, headache, muscle aches, loss of appetite, loss of coordination (ataxia) and chest pain. Almost half of the people have gastrointestinal symptoms and neurological symptoms such as confusion and impaired cognition. Relative bradycardia (low or low-normal heart rate) may also occur.
The people who have Pontiac fever also experience fever and muscle aches without pneumonia. They usually get better within 2-5 days without any treatment. For Pontiac fever, the time between exposure and symptoms is typically a few hours to 2 days.
Diagnosis
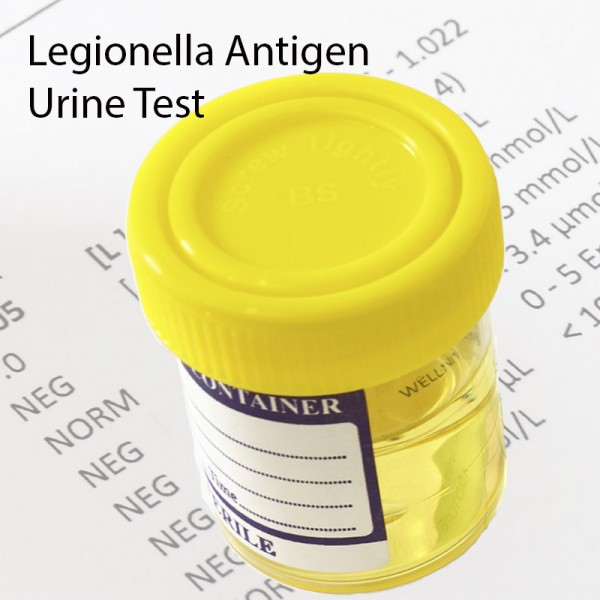
The diagnosis of legionellosis is carried out by a urinary antigen test and sputum culture. The urine antigen test is reliable and detects Legionella pneumophila serogroup 1 only (cause of 70% cases). The laboratory tests may be carried out to check if liver or kidney functions and electrolyte levels are normal or not. This may include low sodium in the blood.
Some of the diagnostic tests that are carried out include detection of bacteria in coughed up mucus, Legionella antigens in sample or urine and comparing Legionella antibody levels in two blood samples (taken in 3-6 weeks’ difference). The chest X-rays may be conducted as they often help in demonstrating pneumonia with consolidation in the bottom portion of both the lungs.
It is often misdiagnosed and it can be hard to differentiate Legionnaires’ disease from other kinds of pneumonia by just looking at the symptoms or radiologic observations. Other diagnostic tests may also be required for confirming the diagnosis.
Treatment & Prevention

No vaccine is available yet for treatment or prevention of Legionellosis. The non-pneumonic form of infection is self-limiting and doesn’t need any medical interventions ushc as antibiotic treatment. However, the patients with Legionnaires’ disease always require antibiotic treatment just after the diagnosis is confirmed. The recommended agents include fluoroquinolones, azithromycin or doxycycline.
The hospitalization is most often required and the death rate is 10%.
The prevention of the disease usually depends largely on implementing water safety plans, good maintenance of water systems, adopting chemical and physical control measures for minimizing bacterial growth, regular cleaning and infecting water sources, and reduce dissemination of aerosols.
Adding biocides to hot and cold water sources to limit growth of bacteria, installing drift eliminators in aerosols especially in hospitals and other health care settings as well as aged-care facilities and reducing stagnant water by flushing unused taps in buildings every week.
Such precautions and others like avoiding ice machines in hospital may help prevent outbreaks and sporadic cases of legionellosis. These control and prevention measures must be carried out under high vigilance by general practitioners and community health services to detect the potential and current cases.
Image Source:
1) phcppros
2) virtual-college
3) bloodtestslondon
4) kostasbeis-tkd