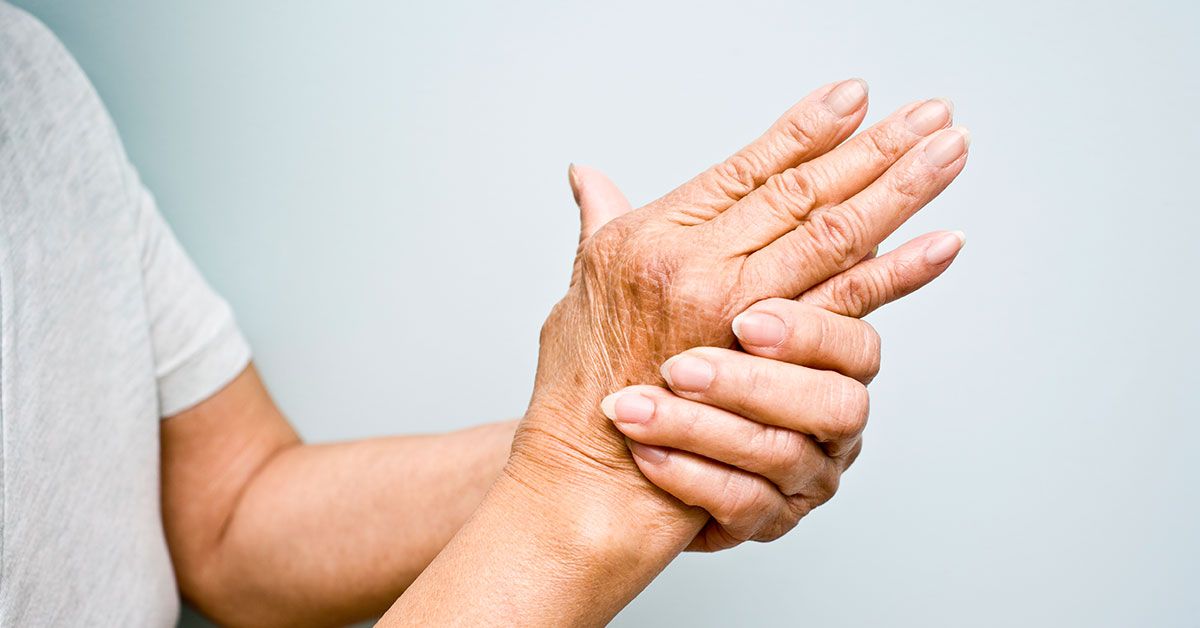
Rheumatoid arthritis (RA) is a chronic autoimmune disease primarily affecting joints and causing their inflammation. The joints on both sides of your body become affected such as both hands, both knees, or both wrists. Such kind of symmetry makes it easier to identify this type of arthritis and rule out others.
Apart from joints, it also affects other body organs such as lungs, eyes, nerves, skin, heart and blood in around 15-20% of the people. Moreover, rheumatoid arthritis affects nearly one-tenth as many people as osteoarthritis.
Here are the signs & symptoms, risk factors & causes, diagnosis, complications and treatment of rheumatoid arthritis.
Symptoms & Signs Of RA
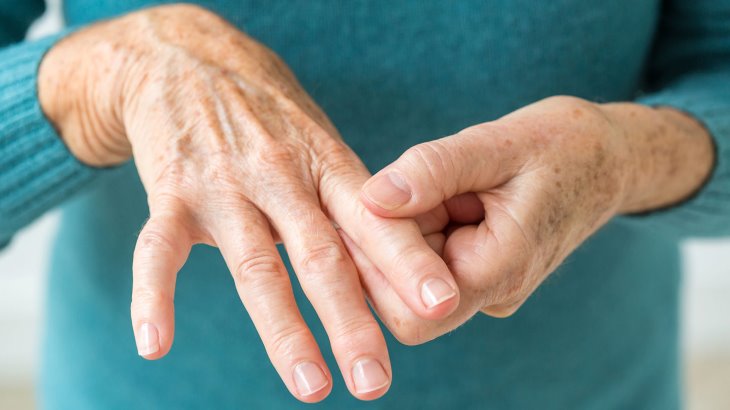
Some of the signs and symptoms that suggest you may have RA:
- Fatigue, fever and weight loss
- Stiffness in joints that worsens in the morning or after inactivity
- Warm, tender and swollen joints
In the early stage, RA affects smaller joints at first especially the joints attaching your fingers to hands and toes to feet. And as the disease increases, the symptoms begin spreading to knees, hips, shoulders, ankles, wrists, and elbows. In most of the cases, symptoms take place in same joints on both sides of body.
The severity of signs and symptoms may vary and come and go. The periods of increased disease activity called flares, alternate with periods of relative remission when the swelling and pain fade or disappear. Over time, RA can lead to deformation and shifting of joints from their place.
Causes & Risk Factors

RA takes place when immune system attacks synovium (linings surrounding the joints). The inflammation causes thickening of synovium that gradually damages the bone and cartilage inside the joint. The tendons and ligaments holding the joint together become weak and stretch. Eventually, the joint undergoes loss in shape and alignment.
The genes do not actually cause RA but they could make you far more vulnerable to environmental factors like viruses and bacteria that cause infection and that may subsequently trigger the disease.
The factors posing risk of RA are:
- Age: Though it can occur at any age, it mostly begins around 40-60 years of age.
- Environmental factors: Asbestos and silica could increase risk of developing RA.
- Obesity: Overweight or obese people are at higher risk of developing RA.
- Cigarette smoking: It could aggravate the disease and increase risk of developing the disease especially if you have genetic predisposition for developing the disease.
- Family history: You are more likely to have RA if a family member had RA.
- Gender: Women have more chances of developing RA than men.
Complications
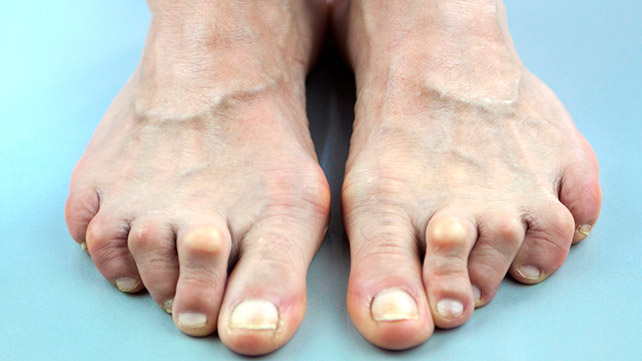
When a person has rheumatoid arthritis, he/she is at a higher risk of having:
-
Infections: The disease as well as the medications used for treating can weaken the immune system, causing increased infections.
-
Lymphoma: Rheumatoid arthritis leads to a higher risk of lymphoma, a group of blood cancers that get developed in the lymph system.
-
Rheumatoid nodules: The firm bumps of tissue mostly form around pressure points, such as elbows. However, these nodules can occur anywhere in the body even lungs.
-
Osteoporosis: Rheumatoid arthritis and certain medications used to treat rheumatoid arthritis may increase your risk of osteoporosis (condition that causes weakening of bones and makes them more susceptible to fracture).
-
Heart issues: The disease may increase risk of having hardened and blocked arteries, as well as inflames the sac enclosing your heart.
-
Lung disease: People with RA tend to have a high risk of inflammation and scarring of the lung tissues and this can cause recurrent shortness of breath.
-
Dry eyes and mouth: People having rheumatoid arthritis are at higher risk of developing Sjogren's syndrome (disorder in which the amount of moisture in your eyes and mouth is reduced).
-
Carpal tunnel syndrome: If you have RA on your wrists, the inflammation can result in compression of the nerve serving most of your hand and fingers.
Diagnosis Of Rheumatoid Arthritis

It may be hard to diagnose RA during early stages as the early signs and symptoms are similar to several other diseases. No physical examination or blood test can help in confirming the diagnosis. In the physical examination, the doctor checks the joints for swelling, redness and warmth. The reflexes and muscle strength could also be examined.
-
Blood tests: People having RA tend to have high erythrocyte sedimentation rate (ESR or sed rate) or C-reactive protein (CRP) that is indicative of inflammatory process in the body. Other common blood tests for rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) antibodies.
-
Imaging tests: X-rays may be recommended for tracking the progression of RA in joints over a period of time. MRI as well as ultrasound tests may help identifying the severity of disease.
Treatment
No cure of rheumatoid arthritis is present. But the recent findings suggest that remission of symptoms have more chances of occurring when the treatment starts early with strong medications called disease-modifying antirheumatic drugs (DMARDs).
When it comes to medications, the types of medications that are recommended depend upon the severity of symptoms and the time duration for which someone had RA.
-
Disease-modifying antirheumatic drugs (DMARDs): These drugs can slow down the advancement of rheumatoid arthritis and prevent the joints and other tissues from permanent damage. The common DMARDs comprise of hydroxychloroquine, methotrexate, leflunomide, and sulfasalazine.
-
Biologic agents: The biologic agents are also known as biologic response modifiers. This newer class of DMARDs comprises of etanercept, rituximab, golimumab, infliximab, abatacept, adalimumab, anakinra, certolizumab, tocilizumab and tofacitinib.
-
NSAIDs or Non-Steroidal Anti-Inflammatory Drugs: These drugs help in relieving pain and reducing inflammation. Over-the-counter NSAIDs include naproxen sodium and ibuprofen. The stronger NSAIDs are prescribed.
-
Steroids: The corticosteroid meds help in reducing inflammation and pain and slow down the joint damage. The doctors often prescribe a corticosteroid for relieving acute symptoms in order to gradually taper off the medication.
These medications target certain parts of immune system which trigger the inflammation and lead to joint and tissue damage. Such types of drugs may even increase infection risk. The biologic DMARDs are generally effective when they are taken along with non-biologic DMARD.
Besides medications, diet changes, practising certain exercises and alternative/home remedies. Low-impact exercises and yoga can improve range of motion of joints and helps in regaining strength and flexibility. Including lot of foods rich in omega-3 fatty acids, antioxidants, fibre and flavonoids in the diet can help in relieving RA. alternative hot and cold treatments are also effective against muscle spasms. Taking rest and getting enough sleep can reduce pain, inflammation and fatigue.