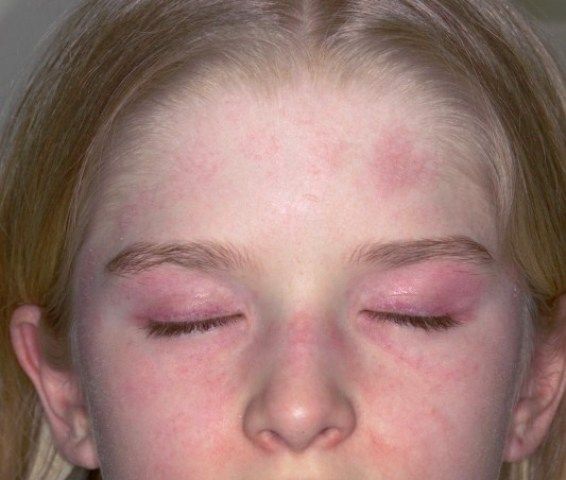
Juvenile Dermatomyositis or JDM is a rare inflammatory disease that mostly affects children of age 5 to 10 years but can also affect people of other ages. This kind of arthritis causes weakening of muscles and skin rash on eyelids and knuckles. Some children may have mild joint symptoms. Remission may be possible but very few children may have a chronic disease.
An idiopathic inflammatory myopathy (IIM) of presumed autoimmune dysfunction, the immune system of the body is believed to attack the blood vessels throughout the body, causing inflammation called vasculitis. Women are more likely to have the condition as compared to men.
Learn about the possible causes, signs and symptoms, diagnosis and treatment of juvenile dermatomyositis.
Causes Of Juvenile Dermatomyositis
The underlying cause of juvenile dermatomyositis is not known. This form of juvenile arthritis is believed to be caused due to anomalies in the immune system of body, leading to inflammation and damage to cells or blood vessels in muscle and skin.
Possibly, it has a genetic component because other autoimmune diseases tend to run in the patient’s families. This disease may be triggered by a condition which causes an immune system activity that doesn’t stop but should. Some common triggers are injuries, infections, sunburn and immunizations.
Signs & Symptoms
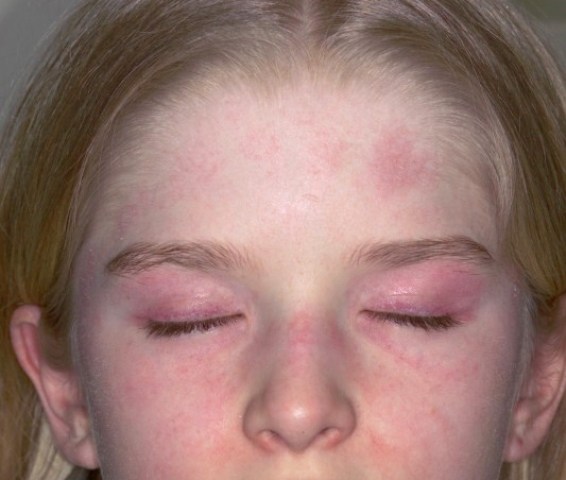
Usually, a red or purplish skin rash on the cheeks or eyelids appears as a first sign. A patchy rash can also be seen near the elbows, nails, back, chest and knees a few weeks/months later. Stomach, back, neck and shoulders mostly feel weak and achy. It may become difficult to run, climb stairs, sit from a lying position and stand up from a seated position.
Dysphonia (weak voice), falling, trouble breathing and dysphagia (difficulty in swallowing) can be other signs. Nearly half of the children having this condition experience muscle pain. Calcinosis and contractures may develop in some children, causing shortened muscles and bent muscles.
It affects both sides of the body and aggravates over time. Fatigue, fever, and weight loss may also occur depending on the body part that is affected. Redness or swelling near the fingernails and skin ulcers (open wounds on skin) may also be seen.
Diagnosis Of JDM

For diagnosing juvenile dermatomyositis, your doctor will look for the presence of characteristic symptoms such as muscle weakness or skin rash. Early diagnosis is crucial for preventing any permanent muscle damage.
The doctor may enquire about the child’s medical history. Some tests which may help in the diagnosis of JDM or in ruling out other conditions include:
-
Blood tests may be conducted for checking the presence of proteins linked with inflammation (autoantibodies) which are related to this condition.
-
Magnetic Resonance Imaging (MRI) is carried out to identify early signs of muscle inflammation and swelling. Powerful magnets and radio waves are used for making a detailed image of the affected areas in the body.
-
Electromyography or EMG measures the electrical activity of child’s muscles and discovers disease location. The small patches are placed on the skin of child and machine connected through wire records the activity.
-
Muscle biopsy for checking signs of infection and inflammation. A small piece of muscle tissue is taken to be checked under a microscope.
-
Nailfold capillaroscopy is a noninvasive test involving putting oil on the skin at the bottom of fingernail. It reveals swelling and changes in capillaries or blood vessels. A lighted magnifying glass helps in detecting active signs of the disease.
Treatment

The treatment goal of juvenile dermatomyositis is reducing inflammation, improving function and preventing further disability. This can be achieved through a combination of medications, physical therapy and speech therapy as well as self-care methods depending on the symptoms.
The medications that are usually prescribed include:
-
Methotrexate gradually reduces inflammation and has lesser side effects than other meds.
-
Corticosteroids are the powerful anti-inflammatory drugs that are often used to treat inflammatory myopathies like JDM as they work quickly. Because of the side effects, they aren’t used for long-term.
-
IntraVenous Immunoglobulin (IVIg) has healthy antibodies from blood donors. They have the ability to block the harmful antibodies attacking the muscle and skin.
-
Other drugs that may be used to treat JDM are azathioprine, tacrolimus, cyclosporine, hydroxychloroquine or anti-TNF therapy.
Other treatments include:
-
Physical therapy: It is done to prevent wasting of muscles, stiffness and contractures. Doing exercises help in maintaining and improving strength and flexibility.
-
Speech therapy: When the throat muscles get weak, speech therapy can help in improving swallowing and speech.
-
Dietary help: Tongue, throat and neck muscles of the child weaken and this makes it hard to swallow and chew the food. Soft foods that are easily chewable should be consumed. Consult a good dietician who can make a proper balanced diet plan. More protein intake may be recommended to aid muscle damage. A feeding tube may be needed if eating process becomes very difficult.
-
Skin protection: Protecting the skin from sun may help in controlling skin disease and potential muscle disease. Apply sunscreen, wear wide-brimmed hats and protective clothing as well as avoid sun exposure during peak hours.