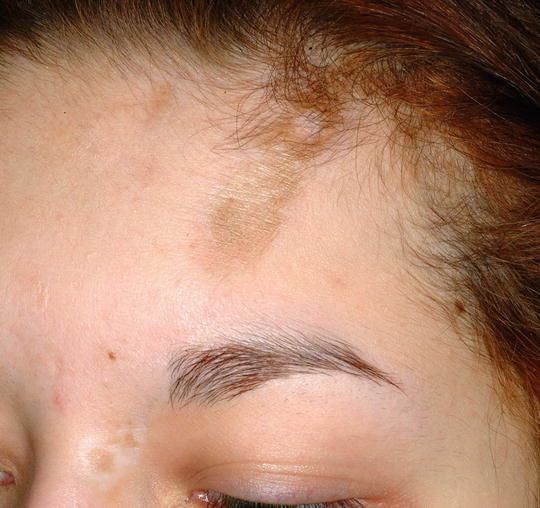
Scleroderma is a group of conditions that causes fibrosis of skin and soft tissues and the term literally means “hard skin”. Juvenile scleroderma is a condition in which the skin becomes unusually hard and thick in children. A form of juvenile arthritis, this rare disease is most common in girls.
Learn about the types, causes, signs and symptoms, diagnosis and treatment of juvenile scleroderma here.
Types Of Scleroderma
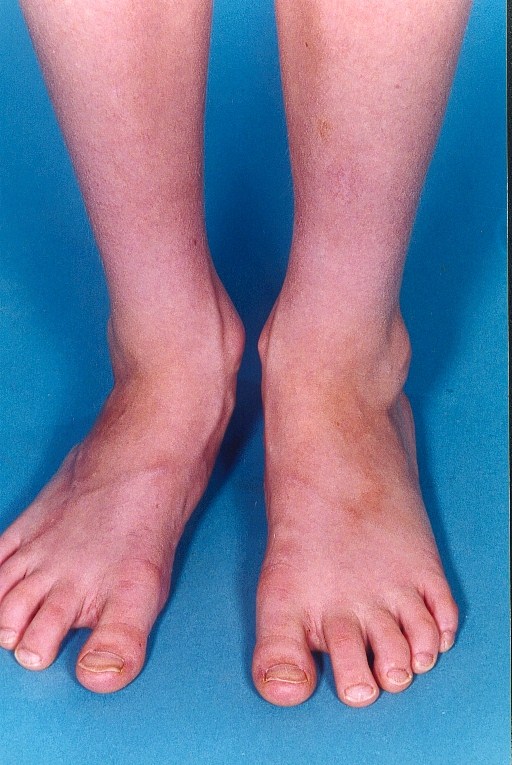
The two forms of juvenile scleroderma include:
-
Localized scleroderma: This type is mostly seen in children. It can be damaging to the skin, muscle, joints and bones. It is unlikely to damage the internal organs.
-
Systemic scleroderma: This form of scleroderma affects the whole body and is rarely seen in children. The internal organs can also become damaged and it can turn severe.
Causes of Juvenile Scleroderma
The exact cause of juvenile scleroderma remains unknown. But researchers believe that these factors may be one of its causes:
-
In localized scleroderma, the immune system mistakenly attacks its own body tissues causing skin inflammation. The connective tissue cells may be triggered to produce excess collagen. The excess collagen can result in fibrosis or hardening and scarring of tissues.
-
Environmental factors such as infections, drug or chemical exposure may trigger the disease.
-
Genetic factors make a child more vulnerable to developing localized scleroderma.
-
In skin injury, wound-healing proteins may be a contributing factor in scleroderma.
A patient having localized scleroderma often have autoimmune conditions like Hashimoto’s thyroiditis, vitiligo (loss of skin pigmentation), and type 1 diabetes. Juvenile localized scleroderma does not decrease a person's life expectancy.
Signs & Symptoms
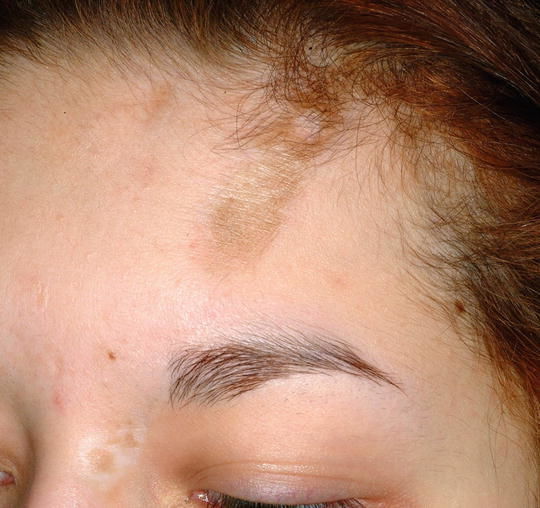
The symptoms of juvenile scleroderma depend on its type. In the localized scleroderma, the skin may turn thickened or thinned, lighter or darker but often appears smooth and shiny. These changes in skin can take place anywhere, from face to arms and legs to trunk in the body.
The two types of localized scleroderma and their symptoms are:
- Morphea:
It is characterized by one or more hard, oval-shaped whitish or darkened skin patches. In most cases, serious long-term complications don’t occur. Morphea can be linear (most common and long plaques appear in lines), generalized (four or more plaques in two or more body areas), bullous (skin blisters or bubbles at the site of plaque and caused due to trauma), deep (rare, most harmful and occurs in tissue under skin) and circumscribed or plaque (least harmful and mainly affects skin in one or two body areas).
- Linear scleroderma:
In this type, lines or streaks of thickened skin are formed over a body area such as leg, arm or head. Deep-tissue injury may be caused. Only one arm or leg is usually affected. The larger areas of linear scleroderma extending over an arm or leg may lead to permanent damage. If not treated properly, permanent changes in arm and leg size may occur. "Scleroderma en coup de sabre" is the term for linear scleroderma crossing the head or face.
Systemic sclerosis is rare in children and it targets the internal organs. Its symptoms affect the skin of fingers, hands, forearms and face. It has more severe long-term effects.
Diagnosis
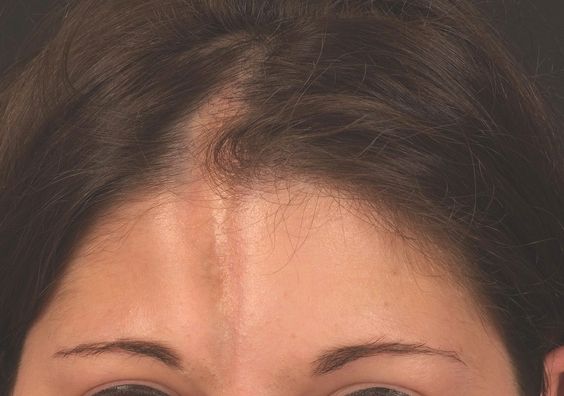
The diagnosis of juvenile scleroderma can be hard as it is a relatively rare condition. It is usually diagnosed based on patient’s history and results of physical examination. No specific lab tests can help in confirming the condition. But tests are often carried out for evaluating inflammation level and ruling out other conditions.
It is often misunderstood for other systemic autoimmune diseases in the early stages. The doctor may:
-
Examine the lesions
-
Ask you to take ultrasound for measuring blood flow through tissues and depth of lesions
-
Carry out infrared thermography for measurement of changes in skin temperature. This helps in determining abnormal areas of tissue growth.
-
Conduct MRI (Magnetic Resonance Imaging) for measuring depth of lesions
-
Suggest a computerized skin score that uses scanned images of skin lesions over time for measuring their dimensions
-
Recommend biopsy of skin or underlying tissue
Treatment
Juvenile scleroderma has no cure. The condition can go into remission but the time may vary. While morphea lesions that don’t extend into deeper tissues may go into remission within a few years, the linear scleroderma lesions can stay active for several years.
The treatment of localized scleroderma is centered on controlling inflammation as this reduces the risk of serious problems. Depending on the degree, topical or systemic treatment is carried out.
The people who have a mild form of this disease are given topical medications for controlling inflammation and softening the skin. These meds consist of calcipotriene, pimecrolimus, imiquimod, corticosteroids and tacrolimus. The moisturizers may help in protecting and softening the skin.
When the large areas have an extreme condition or the disease crosses a joint line and a high risk of permanent damage is there, use systemic medications which suppress the immune system. These meds consist of corticosteroids and methotrexate which are taken as oral medications or intravenous infusion.
Making changes in the diet habits and lifestyle can provide relief to the affected children. Physical therapy and massage can help in improving muscle strength and maintaining joint mobility. Including more Vitamin D in the diet can help. Using skin creams that contain lanolin help in relieving itching and dryness. Phototherapy making use of UV rays can help in softening plaques.
To sum up, physical activity, proper nutrition, skin care and following the doctor’s instructions can improve the condition.
Image Source:
1) pmmonline
2) springernature
3) pinimg
4) vietbao