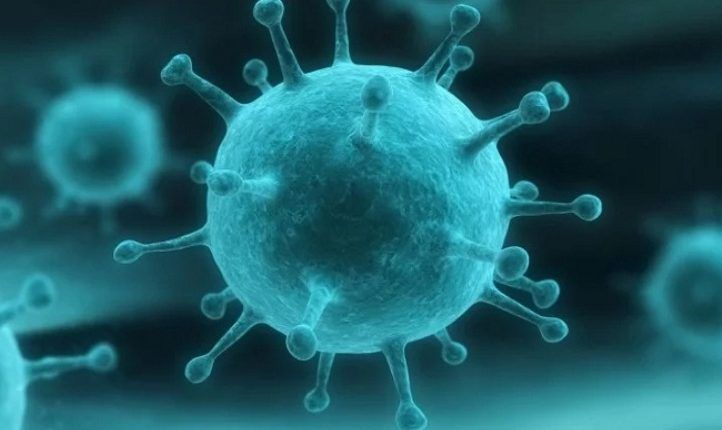
Nipah Virus (NiV) infection is a type of viral infection that is caused by a type of RNA virus in the genus Henipavirus. According to the WHO (World Health Organization), it is an emerging zoonosis that results in severe disease in animals as well as humans. The fruit bats of the Pteropodidae family, Pteropus genus are the natural host of the virus. This infection can spread from person to person and from an animal to a person. The transmission of the disease occurs through direct contact with an infected source.
It can vary from being asymptomatic infection to acute respiratory syndrome and fatal encephalitis. Apart from humans, this virus can affect pigs and other animals. The diagnosis depends on symptoms and is confirmed upon lab tests.
The symptoms can be from none to confusion, fever, headache, cough and shortness of breath. Within a day or two, it may exacerbate into coma. The complications may comprise of inflammation of the brain and seizures following recovery.
Know about its history of outbreaks, risks, symptoms, diagnosis, treatment and prevention here.
History of Outbreaks

It was in 1998 in a village called Kampung Sungai Nipah of Malaysia where Nipah virus infection was first identified during an outbreak and the virus was identified in 1999. The pigs and pig farmers were believed to be infected and were the immediate hosts. So millions of pigs were killed in 1999. But in subsequent outbreaks, no intermediate hosts were there. By the mid of 1999, over 265 human cases of encephalitis including 105 deaths had been reported in Malaysia. Moreover, 11 cases of either encephalitis or respiratory illness with one death were reported in Singapore.
Then in the Meherpur district of Bangladesh in 2001 and Siliguri of India, NiV was reported. In 2004, it was reported in Bangladesh that the humans got infected with Nipah virus after consuming date palm sap contaminated by infected fruit bats. The outbreak also took place in the Naogaon, Manikganj, Rajbari, Faridpur and Tangail districts of Bangladesh in 2003, 2004, and 2005. Bangladesh has witnessed the highest number of deaths and the outbreaks usually occur in the winter season.

Quite recently in May 2018, the outbreak of the disease was reported in the Kozhikode district of Kerala in India. As of 31 May, the number of reported deaths have been 16. These deaths have been recorded mainly in the Kozhikode and Malappuram districts. The infected people have been quarantined as they came into contact with the infected person. Some cases have also been reported in Mangaluru, Karnataka and Himachal Pradesh. Monoclonal antibodies to Nipah virus antigen are being imported from Australia (not yet tested on humans) and Ribavirin tablets from Malaysia.
By 2013, a total of 582 human cases of Nipah virus were estimated and 50-75% of the infected people died. Alos, over 60% of the infection comes from the animals.
Risk Factors
The healthcare workers and hospital caretakers of the infected people are at a high risk of exposure to the virus. In some places like Malaysia and Singapore, the disease has been linked to close contact with the infected pigs. In India and Bangladesh, the virus is believed to occur through the consumption of raw date palm sap (toddy) and contact with bats.
Some experts say that Nipah Virus is an airborne transmission infection and affects people who come in direct contact with the contaminated bodies.
Signs & Symptoms

The signs and symptoms of NiV may take from 3-14 days to appear after the exposure to virus. The initial symptoms are usually not clear and may include headache, fever, drowsiness, nausea followed by mental confusion and drowsiness. It might also be confused with viral fever or common cold. These symptoms may last for upto 7-10 days and result in coma within 1-2 days.
A potentially lethal complication of nipah virus infection is encephalitis (brain inflammation). Also, you must look for any respiratory illness in the early stages. Many patients show neurological, respiratory and pulmonary signs. So these signs should not be ignored.
Diagnosis
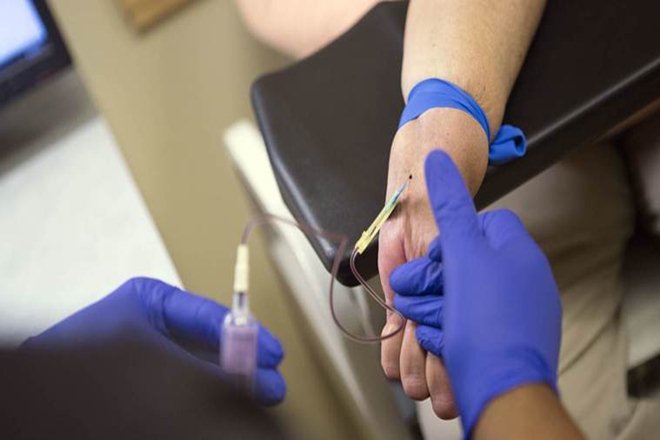
The laboratory diagnosis of Nipah virus infection is carried out using reverse transcriptase polymerase chain reaction (RT-PCR) from throat swabs, cerebrospinal fluid, urine and blood analysis during acute and recovery stages of the disease. The detection of IgG and IgM antibodies can be done after recovery for confirmation of the Nipah virus infection.
Immunohistochemistry on the tissues collected during autopsy also confirm the disease. Viral RNA can be isolated from the saliva of infected people.
Treatment
No specific vaccine or effective treatment is available as yet for animals or humans. The primary treatment for the human cases is intensive supportive care. It is really important to adopt standard infection control practices and proper barrier nursing techniques in order to avoid the transmission of infection from person to person.
All of the suspected cases should be quarantined and should be given intensive supportive care. Ribavirin is found to be effective in vitro tests but it has not yet been proven effective in the humans. The passive immunization using a human monoclonal antibody targeting the Nipah G glycoprotein has been examined in the ferret model as post-exposure prophylaxis.
The antimalarial drug named chloroquine has been demonstrated to block the critical functions required for maturation of Nipah virus. However, no clinical benefit has been observed so far. A human monoclonal antibody ‘m102.4’ has been used on a compassionate use basis in Australia and it is currently in pre-clinical development stage.
Moreover, a subunit vaccine using the Hendra G protein has been found to produce cross-protective antibodies against Nipah Virus in monkeys in order to protect against Hendra virus. However, its potential for use in humans has not been researched so far.
Preventions

It is vital to prevent Nipah virus infection as no effective treatment is there for the disease.
Close observation and awareness are keys to prevent any future outbreaks. Here are some more preventive measures against NiV:
-
This infection can be prevented by avoiding sick pigs and exposure to infected humans and bats in endemic areas.
-
You should also avoid raw palm sap (palm toddy) contaminated by bat excreta, eating fruits partially eaten by bats and water from wells that may be infected by bats. It has been found out that the bats drink toddy accumulated in open containers and sometimes even urinate in it, thereby contaminating it with virus.
-
Taking standard infection control practices should be imposed to prevent nosocomial infections (infection that occur within hospital).
-
The hospitals should bring awareness related to the symptoms and transmission in order to avoid human-to-human infections.
-
Proper diagnosis and tests should be carried out from a recognized facility when the symptoms are experienced.
-
The health professionals who are taking care of infected patients should adopt precautionary measures like wearing masks and gloves.
Image Source:
1) npr
2) thelogicalindian
3) navyamedia
4) indiatimes
5) financialexpress
6) dnaindia
7) ndtvimg