Severe Acute Respiratory Syndrome or SARS is a viral respiratory infection with a zoonotic origin. Caused by the SARS coronavirus (SARS-CoV), it causes flu-like symptoms. A serious form of viral pneumonia, it is a potentially lethal disease that had spread worldwide through unsuspecting travelers in 2003.
The first outbreak of the disease took place in the southern China around November 2002 to July 2003. The disease was identified in February 2003. According to the World Health Organisation (WHO), it is a global health threat and nearly 8098 subsequent cases were reported that resulted in 774 deaths. Majority of the cases were from China (9.6% death rate). Since 2004, no cases of SARS have been reported anywhere in the world.
In the US, 8 lab-confirmed cases without any deaths were reported. All these people had traveled to the areas affected by SARS.
SARS showed how the disease can transmit in a highly mobile and interconnected world. However, high levels of global cooperation helped health experts in quick containment of the disease.
Also in the late 2017, the Chinese scientists traced the virus to cave-dwelling horseshoe bats in Yunnan province.
Read on here to know about the causes, symptoms, diagnosis, prevention and treatment of this illness here.
Causes
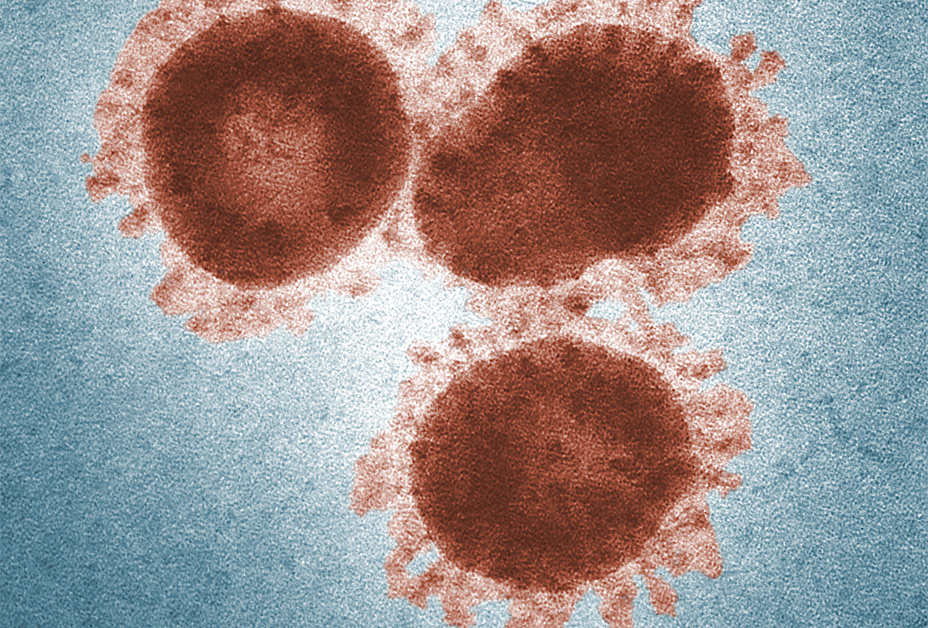
SARS coronavirus is believed to manifest in improperly treated water (waterborne). The disease is caused by a strain of coronavirus (family of virus causing common cold). These viruses have never been specifically dangerous for the humans but they can cause severe disease in animals.
That’s why, the scientists thought that the SARS virus may have passed from animals to humans. And now it appears that it developed from one or more animal viruses into a new strain.
The respiratory droplets from coughing and sneezing and close contact with an infected person may be responsible for transmitting the SARS virus. The respiratory droplets likely absorb into the body via mucus membranes of mouth, eyes and nose.
It can also easily spread through contaminated objects like doorknobs, telephones, elevator buttons, and utensils. The virus can remain active in the environment for many days.
Signs & Symptoms

The symptoms usually appear within 3-5 days after exposure to the SARS virus but they can develop after 2-7 days. During the incubation period, the disease is not contagious before appearance of symptoms.
Most of the cases of SARS begin with symptoms just like flu. These include high fever (more than 100 degrees Fahrenheit), chills, dry coughing, shortness of breath, diarrhea (in 20% cases) and muscle aches. They develop over a course of week.
The symptoms can worsen quickly. Dry cough can be present from 2-7 days during the illness. The cough can prevent your body from getting enough oxygen. And more than 1 in 10 people might need a machine to help with breathing.
SARS can even result in other complications or health ailments such as pneumonia (an infection of the lungs), heart failure and liver failure. The people above 60 years of age who suffer from pre-existing illnesses like diabetes or hepatitis are most likely to have this problem.
Diagnosis
For the diagnosis of SARS, the World Health Organization (WHO) recommends that an individual must show the following:
- Shortness of breath
- A high fever of about 100.4 degrees Fahrenheit
- Radiographic evidence to suggest a diagnosis of pneumonia
- One or more symptoms of lower respiratory tract illness (cough and difficulty breathing)
SARS is a rare illness and its symptoms are similar to pneumonia and flu. A physician will not suspect it unless an individual has been present in the area where the outbreak took place.
These laboratory tests may help in confirming the diagnosis of SARS by identifying the SARS-CoV virus and antibodies.
-
Reverse transcription-polymerase chain reaction (RT-PCR) testing can help in detecting the virus in blood, stool and nasal secretions.
-
Serologic testing can help in detecting SARS-CoV antibodies in the blood. If an individual has antibodies, he or she might also have the infection.
-
The doctors may also use a viral culture. In this process, a small sample of body tissue or fluid can be placed into a container with some cells in which the virus can grow. If the virus is seen to be growing, the cells will change.
These tests may not prove trustworthy if applied in the early stages of infection.
Most of the patients who develop the disease become infected when coming in contact with disease or they had been in places where it was endemic. As pneumonia is a common complication, an individual who develops unexplained pneumonia and has traveled to a place of outbreak or works in lab containing live SARS-CoV should be suspected of SARS.
Treatment
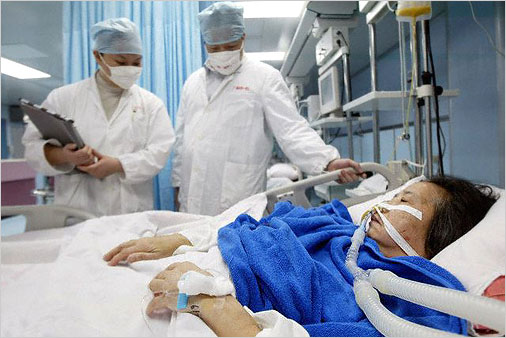
When the outbreak occurred in 2003, it didn’t require people with SARS to go into quarantine but SARS is a reportable disease. It is also a medical emergency and urgent medical care is required.
The WHO advises isolation of patients preferably in negative pressure rooms with use of barrier nursing techniques (filter masks and goggles) to prevent spreading of virus to the healthcare workers. No drugs such as antibiotics appears effective against SARS.
The supportive care is recommended for relieving symptoms (fever and cough). This includes use of medications, antipyretics, mechanical ventilation and supplemental oxygen.
The antibiotics are ineffective as SARS is a viral infection. Some more serious damage caused by SARS may be because of body’s own immune system which reacts in what is called the cytokine storm.
Also, no preventive cure or vaccine is there for SARS that has been shown to be safe as well as effective in the humans. The development of new vaccines and medicines for treating SARS is on-priority for the governments and public health agencies.
A non-profit organization ‘MassBiologics’ is working together with the researchers at NIH and the CDC in developing a monoclonal antibody therapy that showed effectiveness in the animal models.
In 2013, the researchers had informed that they had found a way of disabling a part of the virus involved in SARS which lets it hide from the immune system. This could result in the development of a vaccine against the disease.
Many types of vaccines are being worked upon for SARS but none of them has been tested on humans.
Prevention

Just like other infectious diseases, you can take some simple steps for preventing SARS virus from spreading. A good and effective personal hygiene can help in preventing the spread of SARS virus.
Some of the preventive measures include:
- Washing hands frequently
You should clean your hands often using soap and hot water or you can consider using an alcohol-based hand rub with at least 60% alcohol.
- Wearing disposable gloves
If you come into contact with the person’s body fluids or fecal matter, you must wear disposable gloves. You should throw away the gloves right away after use and wash your hand well.
- Wearing a surgical mask
When you are in the same room as the infected person who has SARS, it is recommended to cover your mouth and nose with a surgical mask. Also, you may wear eyeglasses to get some protection.
- Disinfecting the surfaces
Make use of a household disinfectant for cleaning any surfaces that may have become contaminated with saliva, mucus, sweat, vomit, stool or urine.
- Washing personal items
Using soap and hot water for washing the utensils, towels, bedding and clothing of a SARS-infected person.
Moreover, make sure you avoid touching eyes, nose or mouth with unclean hands. And to avoid spreading infection, cover your mouth while coughing or sneezing and encourage others to do the same.
Do follow these precautions for at least 10 days after the person's signs and symptoms disappear. Keep the children at home from school in case they develop a fever or respiratory symptoms within 10 days of exposure to a SARS-infected person. They may get back to school if the signs and symptoms go away after 3 days.
Image Source:
1. cdc
2. vsebolezni
3. medicalnewstoday
4. pbs
5. cnn

