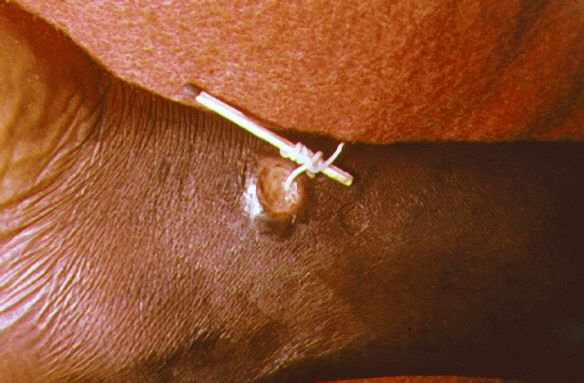
Dracunculiasis, also known by name Guinea worm disease (GWD), is an extremely rare infectious disease. No symptoms are seen at initial stage and the onset of this disease’s symptoms is usually one year after the infection. Categorized under waterborne diseases, it occurs when an individual consumes drinking water containing water fleas contaminated by guinea worms larvae.
Dracunculus medinensis is the only known cause in humans. The female worm causes a painful blister in the skin about a year later and also results in vomiting as well as dizziness. Then a worm emerges from skin, making it hard to work. This condition is unlikely to result in death. Its diagnosis is done on the basis of signs and symptoms.
Know about the causes, symptoms, preventions and treatment of guinea worm disease.
Cause
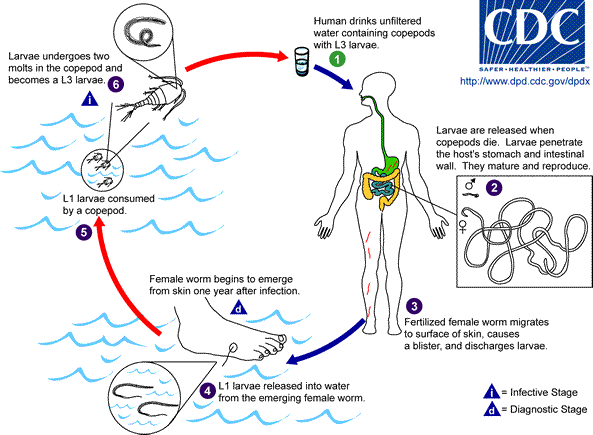
Dracunculiasis is caused by drinking water that is polluted by water fleas hosting the D. medinensis larvae. It is very common in the poorest areas of the world especially where there’s no to limited access of clean water. The still water sources may host copepods carrying the guinea worm larvae.
After ingesting the water, the copepods die, get digested and release stage 3 larvae. These larvae penetrate the host’s stomach or intestinal wall, entering the abdominal cavity and retroperitoneal space. After maturation (nearly 3 months later), the male worm dies and gets absorbed by the body of the infected person.
About one year later, the female worms move to the subcutaneous tissues near the long bones or joints of the limbs. Thereafter, they move toward the surface and cause blisters on the skin usually foot. Within 3 days, the blister breaks and exposes one end of emerging worm. The blister leads to a very painful burning sensation as the worm emerges. When the affected area is submerged in water, the larvae are released in large numbers.
This infection does not create immunity but can occur over and over again during the lifetime. While the disease emerges during the rainy season in drier areas, it is more prevalent during dry seasons in other regions when the water sources are smaller and copepods are more concentrated.
In rare cases, the infection can be caused by eating a fish paratenic host. Reservoir hosts are unknown.
Signs & Symptoms

Draculiasis is detected when emergence of worms is observed from the lesions on the legs of infected individuals. Also, the microscopic examinations of the larvae takes place.
With the worm progressing downward (mostly toward the lower leg) through the subcutaneous tissues, intense pain is caused. Because of the burning sensation that the infected people experience, the disease is known as “fiery serpent”. Some other symptoms include fever, nausea and vomiting.
The female worms lead to allergic reactions and intense burning pain at the time of blister formation while migrating to the skin. These allergic reactions result in rashes, nausea, diarrhea, dizziness and localized edema. When the blister bursts, the allergic reactions reduce. The formation of skin ulcers takes place through which the worm can emerge. The complete healing occurs when the worm is removed. The adult worms’ death in joints can cause arthritis and paralysis in the spinal cord.
Preventions

The guinea worm disease spreads only through contaminated water so it can be prevented by taking these simple measures.
The people must be prevented from contaminated water that contains water flea (cyclops) copepod seen in clean water as swimming white specks. Moreover, take these preventive measures:
- Boiling the water.
- Drinking water obtained only from contamination-free sources.
- Filtering the water using ceramic or sand filters.
- Developing new drinking water sources without any presence of parasites and fixing dysfunctional water sources.
- Treating water sources with larvicides in order to kill the water fleas.
- Filtering the drinking water with a fine-mesh cloth filter like nylon so as to remove the guinea worm-containing crustaceans. Alos, a folded regular cotton cloth happens to be an effective filter. A portable plastic drinking straw with a nylon filter has been a popular trend.
Moreover, the people must also be prevented from emerging Guinea worms that enter drinking water sources.
- Protecting the local water sources in order to prevent people the emerging worms from entering your body.
- Immersing emerging worms in buckets of water to reduce the number of larvae in those worms, and then discard that water on dry ground.
- Discouraging all the community members from getting inside the drinking water source.
- Community-level case detection and containment is crucial.
Treatment
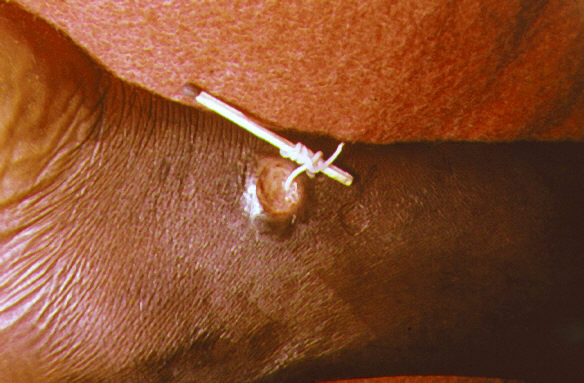
No vaccine or medicine is there for treating the disease. The untreated cases can result in secondary infections, amputations and disability. As soon as the guinea worm starts emerging, you have to carry out a controlled submersion of the affected area in a bucket of water. This causes the worm to discharge hundreds of thousands of larvae into the water, making it less infectious. This contaminated water is then thrown away on the ground far off from the water source. The submersion provides relief in burning sensation and makes worm removal eventually easier.
For extracting the worm, a person is supposed to wrap the liveworm around a piece of gauze or stick. This process may take multiple weeks. A gentle massage of the area near the blister can help in loosening the worm. But if the infection is identified before ulcer formation, the worm can also be removed through medical surgery.
Even though Guinea worm is not fatal in usual cases, the wound where the worm emerges can result in secondary infection like tetanus which can be life-threatening. Analgesics can be used to reduce swelling and pain. Also, the antibiotic ointments can help in preventing secondary infections at the site of wound.
A finding suggests that application of antibiotic ointment on the wound site causes the wound to heal well and quickly but that makes it hard to remove the worm (pulling might break the worm). “Tamale oil” is used for lubricating the worm and helping in its removal.
It is important that the worm does not break while being pulled out. The broken worm tend to putrefy or petrify. The putrefaction causes the skin to drop off around the worm. The petrification occurs when the worm is in a joint or wrapped around a vein or some other important area.
Metronidazole or thiabendazole may also used for making the extraction easier, but it may also may result in migration to other body parts.
Image Source:
1) wikimedia
2) babycenter
3) smugmug
4) wikimedia