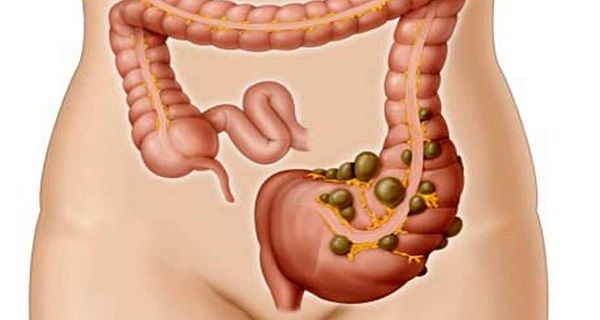
Irritable bowel syndrome (IBS) is a common group of gastrointestinal disorders that usually occur together. This disease is known by many other names including spastic colitis/colon, irritable colon, mucous colitis, spastic bowel. It is a different condition from inflammatory bowel disease (IBD) and is not associated with other bowel conditions.
The symptoms of this condition differ in severity and duration from one person to another. It can cause intestinal damage in certain cases but that’s quite uncommon. It is not life-threatening and does not pose risk of gastrointestinal/colorectal cancer but can still significantly affect your life and can be chronic.
IBS involves trouble with bowel habits and abdominal discomfort or pain. A person may either go more or less often for stools than is normal (diarrhea or constipation) or have abnormal kind of stool (hard, thin, liquid or soft).
Know about the causes, risk factors, triggers, signs, diagnosis, treatment and more of IBS.
Causes
The exact cause of the condition remains unknown but these may be its possible causes:
- Severe bacterial or viral infection
IBS may be developed after a severe attack of diarrhea caused due to bacteria or virus in water or other sources. IBS might be associated with excess bacteria in the intestinal region (bacterial overgrowth).
- Weak muscle contractions in the intestine
The intestinal walls are lined with the layers of muscle which contract while the food moves through the digestive tract. The powerful and long-lasting contractions can lead to gas, bloating and diarrhea. The weak intestinal contractions might slower down the food passage and result in hard, dry stools.
- Inflammation in the intestine
Some people who have IBS have a higher number of immune-system cells in their intestines. This immune-system response is related to pain and diarrhea.
- Bacterial (microflora) changes in the gut
Microflora are the good bacteria living in the intestines are crucial for your health. A study suggests that microflora might be different in people who have IBS as compared to the microflora in healthy people.
- Abnormalities in nervous system
The anomalies in the nerves of digestive system can result in higher discomfort when abdomen stretches from gas or stool. The ill-coordinated signals between the brain and intestines intestines can cause our body to overreact to the changes which usually occur in the digestive process, leading to pain, constipation and diarrhea.
Triggers

The triggers of IBS include:
- Stress
Most of the people having IBS go through aggravated or frequent symptoms at the time of increased stress.
- Hormones
The women have higher chances of having IBS. this may suggest that hormonal changes may be a factor responsible. Many women experience worsened symptoms during their menstrual cycles.
- Food
Though not completely known, IBS symptoms may aggravate due to allergies due to certain foods and drinks like wheat, dairy products, citrus fruits, beans, cabbage, milk and carbonated drinks.
Risk Factors

A lot of people may experience the signs & symptoms of IBS sometimes but you may be at a higher risk due to these factors:
- Age
It is more common in people of age below 50 years.
- Family history
Genetics may be responsible for IBS. The family environment or combination of genes and environment may play a role.
- Gender
Women are more likely to be at the risk of having IBS. Estrogen therapy before or after can be a risk factor.
- Mental health issues
Mental issues such as depression and anxiety are found to have been associated with IBS. a person having history of mental or emotional might also be at risk.
Signs & Symptoms

The most common signs and symptoms of IBS comprise of:
- Excess gas or bloating
- Diarrhea or constipation or (sometimes alternating bouts of both)
- Harder or looser stools
- Bloating
- Mucus in stool
- Cramping, abdominal pain (usually relieved by passing a bowel movement)
Most of the people having IBS do not experience severe signs and symptoms. You must consult a doctor in case of constant changes in bowel habits or other signs/symptoms (it may indicate a more serious condition like colon cancer).
Some of the people also have urinary symptoms and sexual issues. The serious signs and symptoms include:
- Diarrhea at night
- Rectal bleeding
- Difficulty swallowing
- Iron deficiency anemia
- Weight loss
- Unexplained vomiting
- Constant pain
Complications

The chronic constipation or diarrhea may cause hemorrhoids. Moreover, IBS leads to poor quality of life (missing work more frequently or stopping to go to work) and mood disorders (depression, anxiety and others).
Diagnosis
No definite tests exist for diagnosing IBS. The doctor may begin by asking your complete medical history, physical examination and tests for ruling out other conditions. You may also be tested for lactose and gluten intolerance (celiac disease).
Also, blood tests may be conducted to check for anemia and eliminate thyroid problems, and signs of infection.
After ruling out other conditions, your doctor may go for any of these sets of diagnostic criteria:
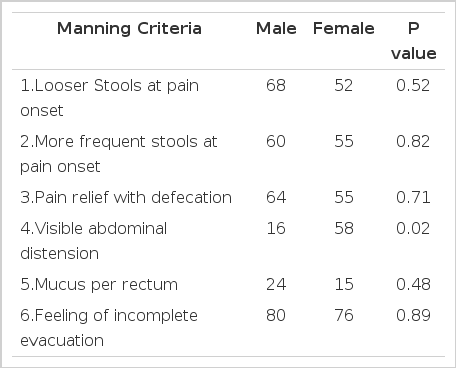
- Manning criteria
These criteria lay focus on the pain relieved by passing stool and having mucus in the stool, incomplete bowel movements, and changes in stool. If the symptoms are more, the chances of having IBS are more.
- Rome criteria
These criteria comprise of abdominal discomfort and pain that last at least one day in a week in three months. It is related to at least two factors: changes in stool consistency, frequency of defecation and pain & discomfort associated with bowel movements.
- Detecting the IBS type
In order to treat the disease, IBS can be categorized into 4 types on the basis of symptoms: diarrhea-predominant (IBS-D), constipation-predominant (IBS-C), mixed (IBS-M) or unsubtyped IBS (IBS-U). Your doctor might check if you have other signs and symptoms (suggesting some other serious condition) like onset after 50 years of age, abdominal pain at night or unrelieved by bowel movement, fever, persistent diarrhea, rectal bleeding, iron deficiency anemia, weight loss, or nausea or recurrent vomiting.
If you have any of these signs or if an initial treatment does not work, you will require more tests. The doctor may recommend various tests such as stool studies to check for any malabsorption. Many other tests can be carried out to rule out other causes of your symptoms.
The imaging tests that may be done include colonoscopy (examining the whole length of colon using a small, flexible tube), X-ray or CT scan (producing images of abdomen and pelvis or conducting barium test/lower GI series) and flexible sigmoidoscopy (examining the lower part of colon using a flexible, lighted tube sigmoidoscope).
The lab tests may include stool tests (stool examination for bacteria/parasites or bile acid in case of chronic diarrhea), upper endoscopy (inspecting upper digestive tract and obtain tissue sample from small intestine & fluid to check for bacterial overgrowth), lactose intolerance tests (inability to produce lactase) and breath tests for bacterial overgrowth (checking bacterial overgrowth in small intestine of people especially those who’ve had bowel surgery, diabetes or condition resulting in slow digestion).
Treatment

The treatment of IBS lays focus on relieving symptoms so that you can live a normal life. The mild signs and symptoms can mostly be controlled through stress management and making diet and lifestyle changes. This may provide you relief. A good dietician can help you with this.
Before going for medications, make adopt of these lifestyle changes:
- Take probiotics (“good” bacteria usually found in the intestines) to help relieve gas and bloating
- Minimize stress (you may try talk therapy)
- Do regular physical exercise
- Cut down on caffeinated beverages that stimulate the intestines
- Eat smaller meals
- Avoid deep-fried or spicy foods
- Avoid smoking
- Take enough sleep
- Drink lots of fluids
- Eliminate high-gas foods, gluten and FODMAPs (fermentable oligo-, di-, and monosaccharides and polyols) from your diet
If you have moderate or severe problems, your doctor may suggest counselling particularly when stress or depression worsens your symptoms.
Apart from this, you should manage your diet. Make sure you modify the amounts or eliminate some foods like dairy, fried foods, indigestible sugars and beans. This may help in reducing various symptoms. In case of some people, adding spices and herbs like ginger, peppermint and chamomile helps in reducing some of the IBS symptoms.
Also, the doctor may suggest medications on depending on your symptoms. It is important to tell the doctor about your current medications including herbal remedies, and over-the-counter medications. This will help the doctor in avoiding medications that might react with what you are already taking.
Certain medications are used for treating all the symptoms, while others are used for relieving particular symptoms. These drugs include medications for controlling muscle spasms, anti-constipation drugs, tricyclic antidepressants for easing pain and antibiotics.
These may include fibre supplements, laxatives, tricyclic antidepressants, anticholinergic medications (dicyclomine), anti-diarrheal medications (loperamide, cholestyramine, colesevelam or colestipol), pain medications (pregabalin or gabapentin) and SSRI antidepressants.
If your major IBS symptom is constipation, linaclotide, plecanatide and lubiprostone are the recommended drugs. And if your major symptoms are diarrhea, Loperamide, Eluxadoline, Bile acid sequestrants and Loperamide can be used. Also, to relieve symptoms of abdominal pain and bloating, antidepressants, antispasmodics and probiotics should be taken.
Moreover, the bulking agents like psyllium, wheat bran, and corn fiber, help in slowing down the movement of food through the digestive system and may also help in relieving the symptoms. The antibiotics like rifaximin can change the amount of bacteria in your intestines. These pills can be taken for 2 weeks, controlling the symptoms for about 6 months.
Prevention

You may look for measures to deal with stress in order to help prevent or relieve symptoms of IBS. You can take counselling, mindfulness training and biofeedback, practice progressive relaxation exercises.
- Biofeedback
The electrical sensors are useful in receiving feedback on your body’s functions. This feedback helps in making some small changes such as relaxing particular muscles in order to relieve symptoms.
- Progressive relaxation exercises
These exercises are effective in relaxing the body muscles. Begin by tightening the muscle in your feet and then slowly relieve the tension.
Now tighten and relax the calves. Keep doing this until your all your body muscles feel relaxed.
- Mindfulness training
It is a technique to reduce stress and allow you to focus on being present in the moment and release all the worries and distractions.
- Counseling
A counselor will help you in learning how to respond to stress. The studies suggest that psychotherapy significantly reduces the long-lasting symptoms.
- Diet management
Avoid large meals, fatty foods, too much fibre, carbonated drinks, dairy products and rather eat moderate amounts of soluble fibre.
Image Source:
1. fullyfunctional
2. nativebars
3. newsapi
4. ibsliving
5. self
6. kjim
7. medsludinfo
8. pinimg