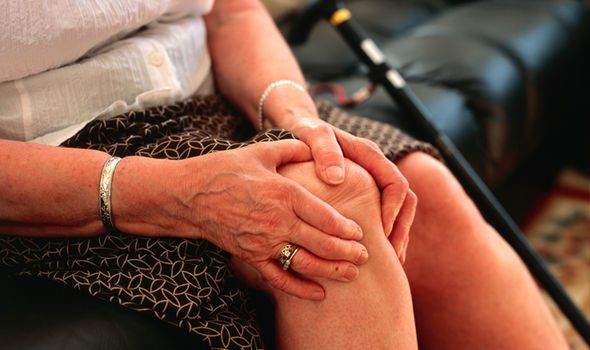
The infectious arthritis, also known as septic arthritis, is a painful infection that occurs in a large joint typically knee, hip or shoulder. This type of arthritis is usually caused by bacteria but can also be caused due to virus or fungi. In some cases, it can affect multiple joints. If its treatment is delayed, it can result in complications such as joint degeneration and permanent damage.
Read about the signs & symptoms, causes, risk factors, diagnosis and treatment of septic (infectious) arthritis.
Causes Of Infectious Arthritis
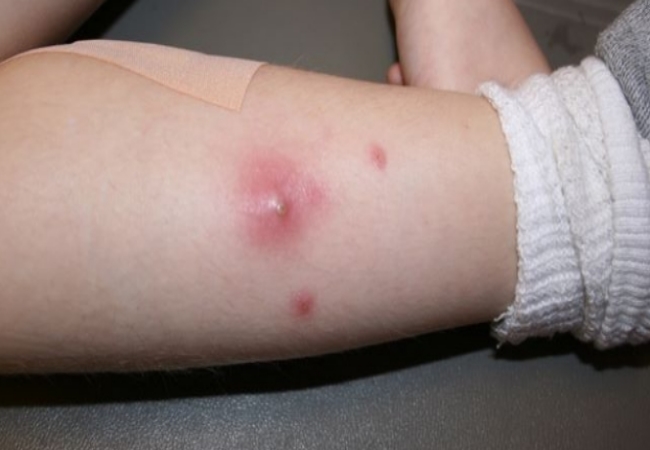
This condition occurs when an infection caused due to bacteria, virus or fungi begins in another area of the body (skin infection or urinary tract infection) and spreads through bloodstream to a joint or the fluid (synovial fluid) around the joint. This infection may also come through open wounds, surgery, or injections.
The infection may also enter the body through an opening from surgery (like knee surgery), drug injections or open wounds that deliver germs directly into the joint. The synovium or the lining of your joints is nearly unable to protect itself from the infection. The body’s reaction to the infection, including inflammation that can increase pressure and decrease blood flow inside the joint, can further the damage.
In the adults as well as children, the common bacteria causing acute septic arthritis include staphylococcus aureus (staph) and streptococcus. These foreign invaders enter the bloodstream and infect the joint, causing pain and inflammation.
The virus infections that cause this kind of arthritis include HTLV-1, Herpes viruses, Mumps, Coxsackie viruses, Parvovirus B19, Adenovirus, HIV (AIDS virus) and Hepatitis A, B, and C. The fungi causing infectious arthritis include coccidiomycosis, blastomyces and histoplasma. These infections tend to develop slowly as compared to bacterial infections.
Risk Factors

Most commonly, the children, older adults and people using illegal drugs are affected by septic arthritis. And in most common cases, knees are affected but shoulders, hips and other joints are also affected.
Immediate treatment is required as the infection may quickly and severely damage the cartilage and bone inside the joint.
The presence of any one or more of these risk factors causes infectious arthritis:
-
Existing joint problems: The chronic diseases affecting your joints, such as osteoarthritis, gout, rheumatoid arthritis or lupus, pose risk of having septic arthritis. Moreover, an artificial joint or previous joint surgery and joint injury also increase the risk.
-
Skin fragility: The skin that easily breaks and heals poorly can allow bacteria to enter your body. The infected skin wounds as well as skin conditions like psoriasis and eczema increase the risk of septic arthritis. The people injecting drugs on a regular basis also have a higher risk of infection.
-
Joint trauma: The animal bites, puncture wounds or cuts over a joint can increase the risk of having septic arthritis.
-
Weak immune system: The people having a weak immune system are at higher risk of septic arthritis. These include diabetics, people having kidney and liver problems and those who take drugs which suppress their immune systems.
-
Rheumatoid arthritis medications: People suffering from rheumatoid arthritis have a an increased risk of having infectious arthritis as these medications can suppress the immune system and infections are more likely to occur. The diagnosis of septic arthritis in people with rheumatoid arthritis is hard as their various signs and symptoms are similar.
Symptoms of Septic Arthritis
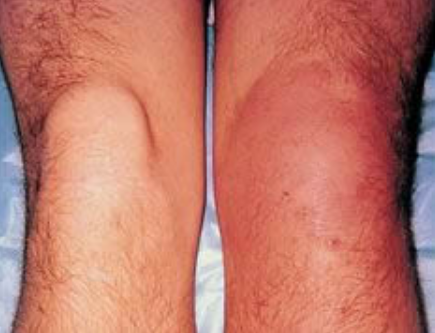
The signs and symptoms of infectious arthritis depend on the age and medications you take. Some of the common ones include:
-
Extreme discomfort
-
Intense pain in the affected joint that aggravates with movement
-
Chills
-
Fatigue and generalized weakness
-
Fever
-
Redness, swelling (increased fluid inside the joint) and warmth (increased blood flow) in and around the joint
-
Difficulty in moving limb with the affected joint
-
Irritability
-
Decreased appetite
-
Rapid heart rate
Diagnosis
For the diagnosis of infectious arthritis, following procedures and tests are carried out:
-
Arthrocentesis (joint fluid analysis) is a commonly used test procedure for correct diagnosis of septic arthritis. It involves a surgical puncture of joint for withdrawing a sample of joint fluid called synovial fluid. This fluid is usually sterile and acts as a lubricant. The infections can alter the consistency, volume, color and composition of fluid in joints. The lab test help in determining what is causing the infection and which meds should be prescribed.
-
Blood tests will help in finding out if there’s any sign of infection in the blood. A blood sample is taken from the vein using a needle.
-
Imaging tests like X-rays as well as CT (computer tomography), MRI and nuclear scans are useful in determining the amount of damage in the joint.
Treatment

The doctors typically rely antibiotic drugs and joint drainage for the treatment of septic arthritis.
- Antibiotics
For choosing the right and the most effective medication, the doctor needs to identify the microbe that is the cause of the infection. The antibiotics are typically administered through a vein in the arm at first. Later on, oral antibiotics may be used.
The antibiotic treatment usually lasts from 2-6 weeks. Ask your doctor about the side effects that can be expected from the medication.
- Joint drainage
The infected joint fluid must be removed. The various joint drainage methods include:
1. Needle inserted in the joint can help the doctor in withdrawing the infected fluid.
2. Scope procedure: In the arthroscopy, a flexible tube having a video camera at its tip is placed in your joint by making a small incision. Suction and drainage tubes are then inserted through small incisions around your joint.
3. Open surgical procedure may be carried out when it’s difficult to drain the fluid using a needle or arthroscopy in some joints, such as the hip.
In certain cases, surgery is required for removal of any damaged sections of the joint or for replacement of the joint. However, this is only done after the infection treatment.
Other treatment methods for reducing the pain that are used along with treatment for the infection include using nonsteroidal anti-inflammatory drugs (NSAIDs), resting the joint, splinting the affected joint and taking physical therapy.
Image Source:
1) findarthritistreatment
2) netdna-ssl
3) imimg
4) mims
5) findarthritistreatment