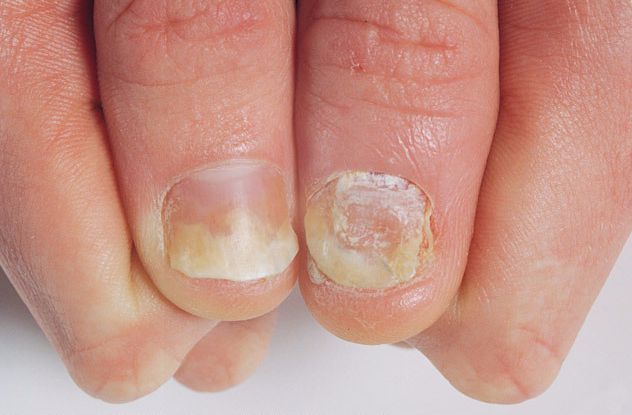
Psoriatic arthritis is a type of arthritis that affects people suffering from psoriasis as well as arthritis. This causes inflammation of skin and joints. In this condition, red patches of skin topped with silvery scales are seen.
In most cases, people develop psoriasis first and are later detected with psoriatic arthritis. The joint problems can, however, begin before skin lesions become visible. This chronic autoimmune disease often affects knee and elbow tips, navel, scalp and ears, and areas around the crotch. Nearly 15-25% of patients having psoriasis also develop an associated joint inflammation. Also, people with inflammatory arthritis and psoriasis are diagnosed with psoriatic arthritis.
Read on here to know about the different types, risk factors, causes, signs and symptoms, complications, diagnosis, and treatment of psoriatic arthritis.
Different Types Of Psoriatic Arthritis
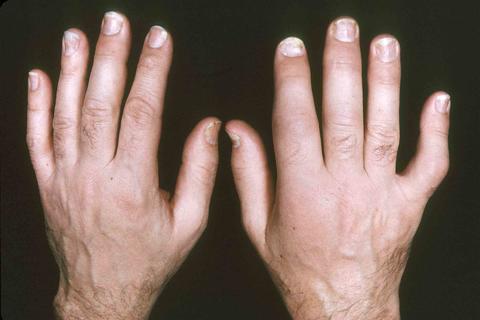
The 5 main types of psoriatic arthritis are as below:
- Asymmetric psoriatic arthritis (Oligoarticular)
This type of psoriatic arthritis affects nearly 70% of patients and is usually mild. It does not affect the same joints on both sides of the body and typically involves fewer than three joints: knee, hip and one or many fingers.
- Symmetric psoriatic arthritis (Polyarticular)
This type of psoriatic arthritis occurs in nearly 25% of patients and affects five or more joints on both the sides of the body simultaneously. It is very similar to rheumatoid arthritis and is disabling in about 50% cases.
- Arthritis mutilans
This is a rare type of psoriatic arthritis affecting less than 5% of the patients. A severely destructive and deforming arthritis, it can progress over months or years and causes severe damage of joints. It is also known as chronic absorptive arthritis and is frequently associated with neck and lower back pain.
- Spondyloarthritis
This type of psoriatic arthritis is characterized by inflammation and stiffness of the neck or the sacroiliac joint of the spine. But it can also have an influence on the hands and feet, just like is the case with symmetric arthritis.
- Distal interphalangeal predominant (DIP)
This type of psoriatic arthritis occurs in nearly 5% of patients and is characterized by inflammation and stiffness in the joints closest to the ends of the fingers and toes. Often confused with osteoarthritis, the nail changes are often smeared.
Signs & Symptoms
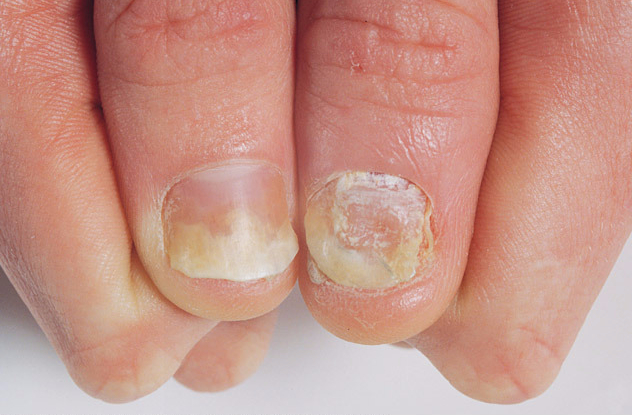
As psoriatic arthritis is a chronic disease, it aggravates with time but sometimes its symptoms may either improve or reduce in intensity alternating with times when the symptoms worsen.
Psoriatic arthritis may affect the joints on one side (asymmetric) or both sides of the body (symmetric). Its signs and symptoms are very similar to rheumatoid arthritis. Both the diseases cause pain and swelling in joints and are warm to touch.
Moreover, psoriatic arthritis also leads to
-
Lower back pain: Spondylitis may be caused in some people due to psoriatic arthritis. And this usually causes inflammation of joints between vertebrae of spine and joints between spine & pelvis.
-
Swollen fingers and toes: This condition can lead to painful, sausage-like swelling of your fingers and toes. Swelling and deformities in your hands and feet may even develop before any crucial joint symptoms.
-
Foot pain: This type of arthritis can also lead to pain at the points where tendons and ligaments attach to your bones, especially at the back of your heel (Achilles tendinitis) or in the sole of your foot (plantar fasciitis).
Causes
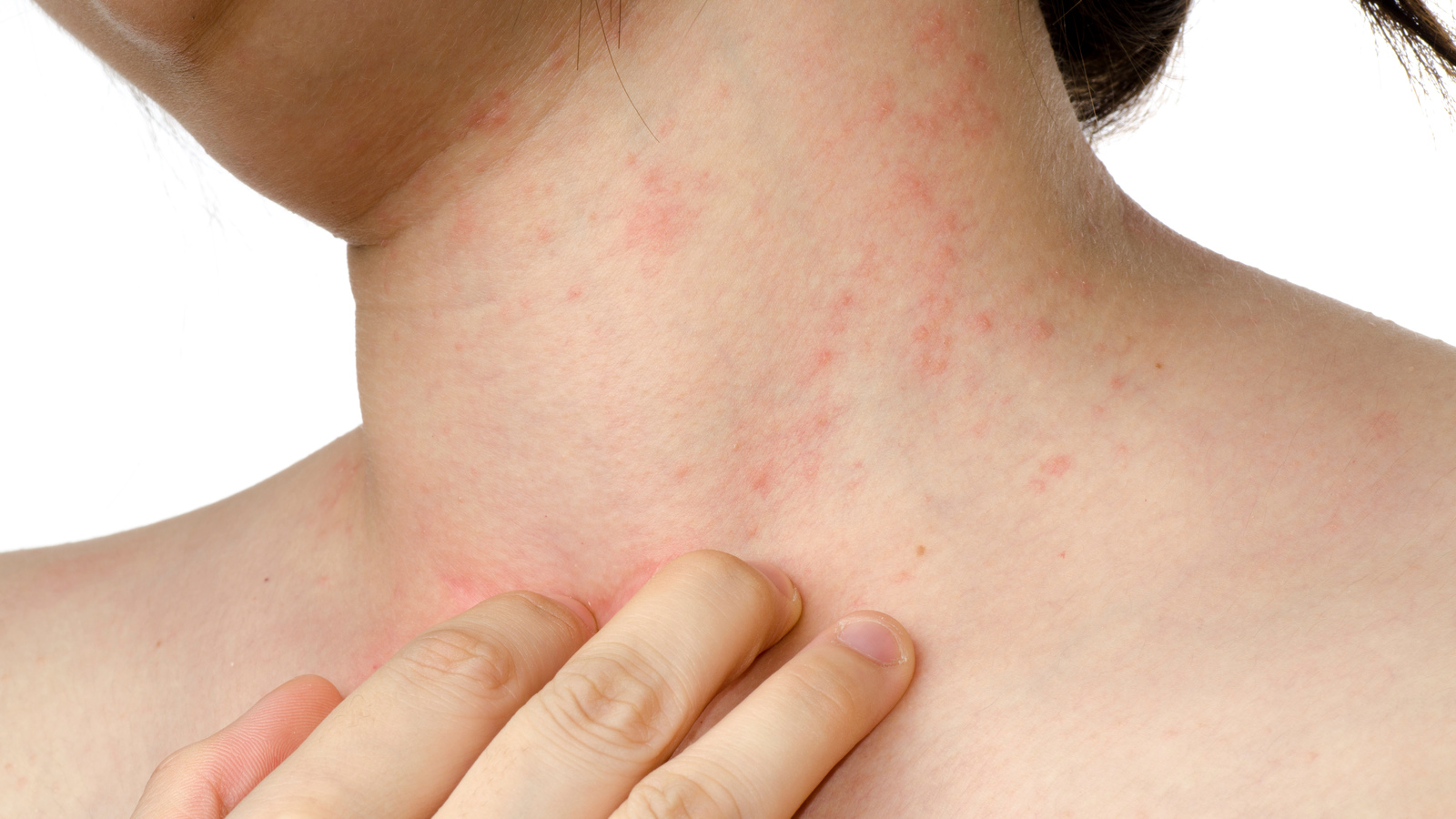
The psoriatic arthritis is caused when the immune system of your body starts attacking healthy cells and tissues. The abnormal immune response leads to inflammation in joints and overproduction of skin cells.
Several people having psoriatic arthritis have a family history of psoriasis or psoriatic arthritis. The researchers have found certain genetic markers that seem to have a link with psoriatic arthritis.
Physical trauma or an environmental factor such as viral or bacterial infection may trigger psoriatic arthritis in those who have an inherited tendency.
Risk Factors
The various factors that add to the risk of having psoriatic arthritis include:
-
Family history: A lot of people having psoriatic arthritis have some family member having this disease.
-
Age: Even though can develop psoriatic arthritis in anybody, it’s most common in adults around 30-50 years of age.
-
Psoriasis: The biggest risk of developing psoriatic arthritis is psoriasis. The people having psoriasis lesions on nails are more likely to develop it.
Other triggers or risk factors include streptococcal infections, smoking, HIV, certain drugs, alcohol, emotional stress, hormonal changes, sunlight and skin injury.
Complications
Few people having psoriatic arthritis develop arthritis mutilans which is a severe, painful and disabling form of the disease. Over time, this deteriorates the small bones in your hands especially fingers causing disability and permanent distortion.
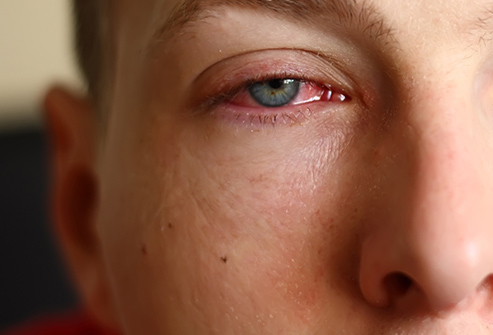
People having psoriatic arthritis sometimes also develop eye problems like pinkeye (conjunctivitis) or uveitis which can lead to red, painful eyes and blurry vision. They are also at a higher risk of having cardiovascular disease.
Diagnosis

At the time of physical examination, you doctor will do/look for following:
- Checking fingernails for flaking, pitting and other aberrations
- Pressing on soles of feet and around heels for finding tender areas
- Examining the joints closely for signs of tenderness and swelling
There’s no single test that can help in confirming diagnosis of psoriatic arthritis. However, some tests can rule out other causes of joint pain like rheumatoid arthritis or gout.
The imaging tests carried out include:
- X-Rays
Plain X-rays help in pointing out changes in the joints that only take place in psoriatic arthritis but not in other arthritic conditions.
- Magnetic resonance imaging (MRI)
MRI makes use of radio waves and a strong magnetic field for producing highly detailed images of both hard and soft tissues in your body. Such kind of imaging test may be used for checking issues with the tendons and ligaments in your feet and lower back.
The two laboratory tests conducted are:
- Joint fluid test
A doctor removes a small sample of fluid from an affected joints mostly knee using a needle. The crystals of uric acid in joint fluid may suggest that you have gout and not psoriatic arthritis.
- Rheumatoid factor (RF)
RF is an antibody that is often found in blood of those having rheumatoid arthritis but not in blood of those having psoriatic arthritis. So this test helps the doctor in differentiating between the two conditions.
Treatment
There’s no cure for psoriatic arthritis and its treatment lays focus on control of inflammation in affected joints for preventing pain and disability.
The medications or drugs used for treating psoriatic arthritis are:
-
Immunosuppressants are the meds that controls your immune system which becomes out of control in psoriatic arthritis. Some of the examples include azathioprine and cyclosporine. These meds can help in increasing your susceptibility toward infection.
-
NSAIDs or Nonsteroidal anti-inflammatory drugs can help in relieving pain and reducing inflammation. Over-the-counter NSAIDs include ibuprofen and naproxen sodium. Stronger NSAIDs are made available on doctor’s prescription.
-
TNF-alpha or Tumor necrosis factor-alpha inhibitors reduce the pain, stiffness and tender or swollen joints. Some of these include etanercept, infliximab, adalimumab, golimumab and certolizumab.
-
DMARDs or Disease-modifying antirheumatic drugs help in slowing down the progress of psoriatic arthritis and in preventing joints and other tissues from permanent damage. The common DMARDs include leflunomide, sulfasalazine and methotrexate.
-
Newly developed medications for plaque psoriasis can also help in reducing the signs and symptoms of psoriatic arthritis. Some examples include apremilast, ustekinumab and secukinumab.
Other procedures that help relieve this condition include steroid injections and joint replacement surgery. This can reduce the inflammation quickly and is sometimes injected into the affected joint. In joint replacement surgery, the joints that are severely damaged by psoriatic arthritis can be replaced using artificial prostheses made out of metal and plastic.
image Source:
1. health
2. mayoclinic
3. psoriasisfreetips
4. healthline
5. webmd
6. agoramedia
7. agoramedia